Nutrition
Americans are living longer than ever and good nutrition and physical activity are essential to reducing the risk of chronic disease and disability. Most Americans consume more calories than they expend, and their diets contain too much saturated fat, sugar and sodium, and inadequate amounts of fruits, vegetables, whole grains, calcium and fiber. As a consequence, body weight and fat increase with age. Many Americans also become less physically active as they age. Reductions in physical activity with age are associated with reduced muscle and bone mass. Fortunately, healthy eating and adequate physical activity as part of a healthy lifestyle can reduce risk of chronic disease and disability and improve quality of life.
Four key points about nutrition to keep in mind as we age:
1 | Calorie and Protein Needs Change with Age
Calorie needs decline with age due to changes in body composition and reductions in physical activity levels. These changes result in a reduction in metabolic rate and the number of calories that are needed each day. The body’s ability to digest and use dietary protein to maintain and build muscle also declines with age. Because of these and other changes, most people experience a reduction in muscle mass and strength with age—termed sarcopenia—which is associated with a decline in the ability to perform daily activities and disability.
TIPS to MANAGE CHANGING CALORIE AND PROTEIN NEEDS
Engage in regular physical activity. The American College of Sports Medicine and Centers for Disease Control recommend 150 minutes per week of moderate physical activity (walking, swimming), 75 minutes per week of vigorous physical activity (jogging, cycling) or a combination of both moderate and vigorous physical activity.
Consider resistance or strength training. Talk with your doctor about beginning a regular resistance or strength training routine to help minimize loss, maintain or even increase muscle mass.
Eat protein throughout the day. Consuming 25 to 30 grams of protein at breakfast, lunch and dinner can be helpful in maintaining muscle mass and function. Lean meats, fish, low-fat dairy, soy products, eggs, beans and nuts are all excellent sources of protein (4 ounces of chicken contains 30 grams of protein; 1 cup of Greek yogurt contains 17 grams of protein).
Eat more fruits and vegetables. Eat a variety of high-volume, lower-calorie foods—like raw and cooked vegetables and whole fruits—to reduce calories and feel satisfied after a meal.
2 | Changes in Bone Mineral Density
Peak bone mass is reached around age 25 to 30. The body’s ability to turn over old bone and make new bone declines with age, leading to a decline in bone density. For women, the rate of bone loss increases in the years surrounding menopause. For both sexes, but particularly women, taking action to ensure maintenance of adequate bone mineral density is important for avoiding the increased risk of falls and fractures.
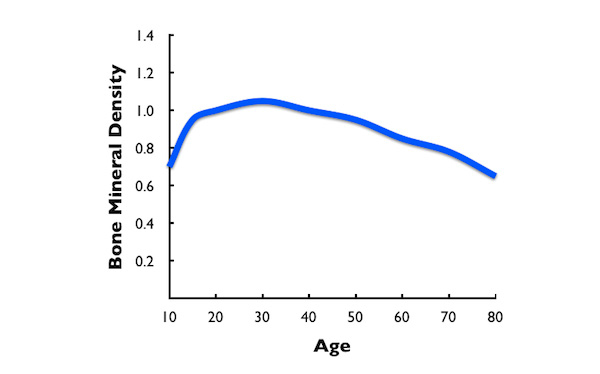
TIPS to MAINTAIN BONE MINERAL DENSITY
Eat foods rich in calcium and vitamin D (like low fat milk and dairy products, tofu and dark, leafy greens).
Look into vitamin D. Talk with your doctor about taking a vitamin D supplement.
Consider resistance or strength training. Talk with your doctor about beginning a regular resistance or strength training routine.
3 | Changes in Digestion and Absorption
As with other body systems and organs, digestive systems may become less efficient in absorbing key vitamins (including vitamin B12) with aging. In addition, the movement of foods through the stomach and large intestines may decrease, potentially resulting in constipation. Getting enough fluids and fiber can help improve digestive motility.
TIPS to MAINTAIN DIGESTION, ABSORPTION AND METABOLISM FUNCTIONS
Drink your fluids. Drink plenty of non-caloric fluids, such as water, throughout the day.
Eat fiber-rich foods like whole fruits, vegetables, beans and whole grains to achieve a goal of getting 20 to 25 grams per day.
Get enough vitamin B12. Talk with your doctor about your vitamin B12 levels and whether or not you need a vitamin B12 supplement.
4 | Changes in Fluid Balance
In an aging body, the mechanisms that keep fluids and electrolytes in balance become less effective. As a result older adults are more likely to become dehydrated than younger adults. In addition, certain medications (diuretics) can alter the way the kidneys function to regulate fluids and electrolytes. Because so many body processes require water—including digesting and transporting nutrients throughout the body, and excreting toxic waste products—regulating body temperature and maintaining adequate fluid balance is critical.
TIPS to MAINTAIN FLUID BALANCE
Eat foods that contain fluids (like soups and stews).
Drink water throughout the day, not just at mealtime.
Drink a variety of hot and cold beverages (hot and cold tea, coffee, low-fat or skim milk), but limit the fruit juices and sugar sweetened beverages as these can add unnecessary calories.
About the Experts

Mary Elizabeth Baugh, M.S., R.D., received her B.S and M.S. degrees in the Department of Human Nutrition, Foods, and Exercise at Virginia Tech. She is a Registered Dietitian with extensive experience in weight management settings. Ms. Baugh is currently a doctoral student at Virginia Tech.

Kevin P. Davy, Ph.D., received his Ph.D. in Applied Physiology at Virginia Tech and completed his postdoctoral training in Integrative Physiology at the University of Colorado. He has served on the faculties of Colorado State University and the University of Mississippi Medical Center. Dr. Davy is currently Professor and Director in the Department of Human Nutrition, Foods, and Exercise and the Fralin Translational Obesity Research Center at Virginia Tech. His research interests are focused on the etiology, prevention and treatment of the cardiometabolic sequalae of obesity and aging.